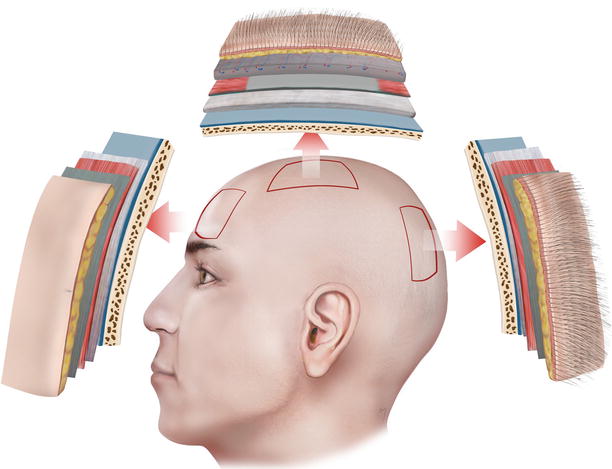
Central Centrifugal Cicatricial Alopecia
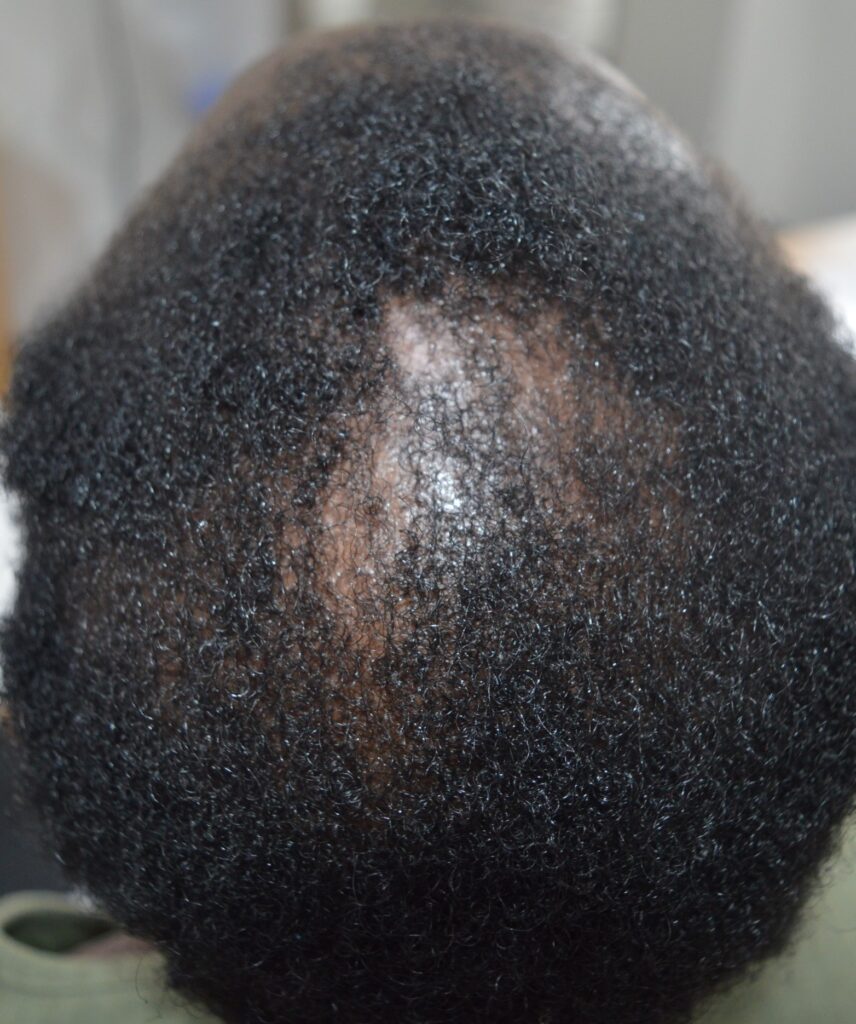
Central centrifugal cicatricial alopecia (CCCA) is a type of scarring hair loss which usually starts on the scalp vertex and spreads outwards. It is the most common form of scarring alopecia seen in women of African descent, with a typical age of onset of 30-40 years.
What causes central centrifugal cicatricial alopecia?
The cause of CCCA is not fully understood but may be related to the following factors:
- A mutation in the PADI3 gene has been found in some patients with CCCA
- Traumatic hair care practices e.g., hair straightening using hot combs and chemical relaxers, tight hairstyles, braids and weaves are thought to be risk factors but the link is controversial
- Increased tendency to develop fibrosis (scarring) e.g., keloid scars and uterine fibroids
- Possible association with type 2 diabetes mellitus
What are the symptoms and signs of central centrifugal cicatricial alopecia?
Often there are no symptoms. However, some patients may experience itching, burning, tingling, or tenderness.
Hair breakage may precede scarring hair loss. Central centrifugal cicatricial alopecia typically begins on the scalp vertex and spreads outwards (described as a centrifugal pattern). The affected areas may have a shiny appearance.
How is central centrifugal cicatricial alopecia diagnosed?
Central centrifugal cicatricial alopecia can often be recognised by its characteristic appearance and distribution. However, if the diagnosis is uncertain, a biopsy may be performed.
How is central centrifugal cicatricial alopecia treated?
The treatment of CCCA may include:
The treatment of CCCA may include:
- Avoidance of traumatic hair grooming practices
- Topical, intralesional or oral corticosteroids
- Topical calcineurin inhibitors
- Topical minoxidil
- Low-dose oral minoxidil
- Doxycycline
- Antimalarial drugs e.g., hydroxychloroquine
- Systemic immunosuppressants e.g., ciclosporin and methotrexate
- Hair transplantation if condition has been stable for 1-2 years
Dissecting Cellulitis of the Scalp