Psoriasis
Psoriasis is a common skin disease affecting 2% of the population. It occurs equally in men
and women and can begin at any age. Psoriasis is a long-term condition which may
intermittently flare up throughout one’s lifetime. Psoriasis commonly affects the scalp. It
can affect the nails and the joints as well as the skin.
Psoriasis, particularly moderate-to severe-psoriasis, is associated with an increased risk of
anxiety, depression and harmful use of alcohol. Moderate-to-severe psoriasis increases the
risk of heart disease and stroke and treatment of psoriasis may reduce this risk. Psoriasis can
also be associated with diabetes, obesity, inflammatory bowel disease, venous
thromboembolism, high cholesterol and hypertension.
What causes psoriasis?
Both genetic and environmental factors play a role in the development of psoriasis.
Infections, stress, damage to the skin and alcohol may trigger flares of psoriasis. Certain
medications e.g., β-blockers and lithium can trigger flare-ups of psoriasis, whereas sudden
discontinuation of oral corticosteroids can trigger or worsen psoriasis. Obesity and smoking
are associated with a poor response to treatment. Psoriasis is more common in patients
with a positive family history. The mode of inheritance is complex and not completely
understood.
What are the symptoms and signs of scalp psoriasis?
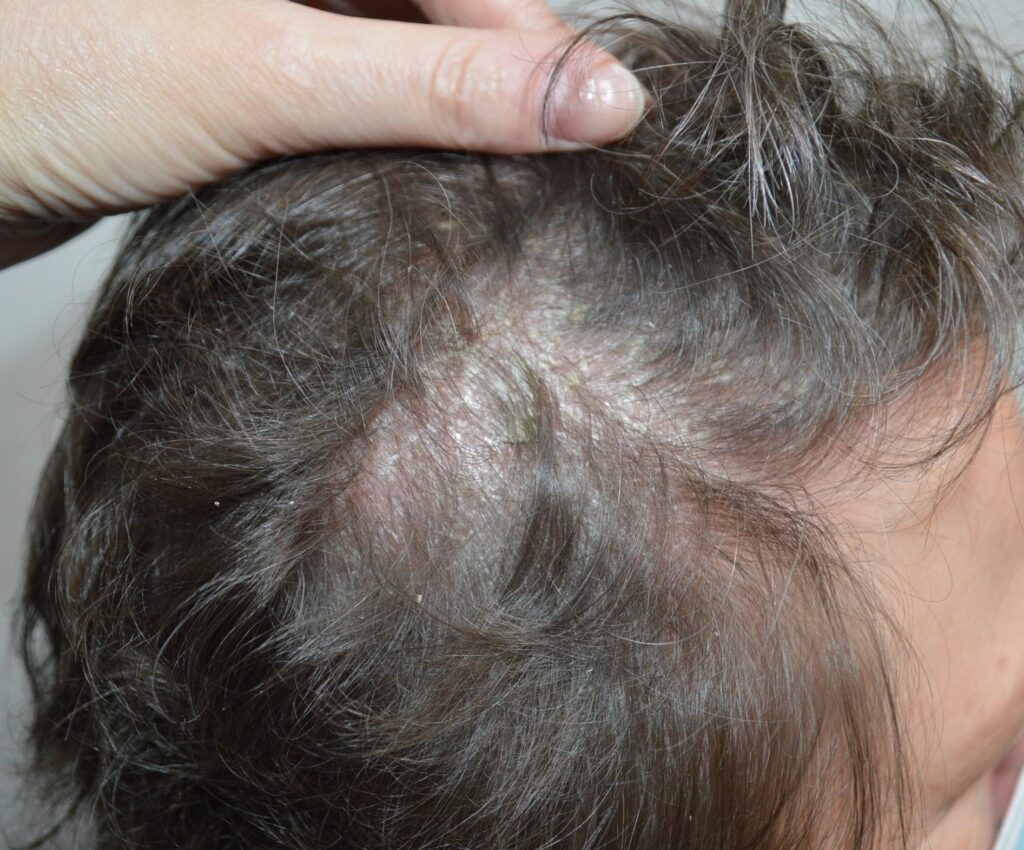
Psoriasis may not have any associated symptoms, although itching can occur. The scalp can
be particularly itchy. Psoriasis causes well-defined and slightly raised pink or red areas with
silvery-white scales (known as ‘plaques’). Many people have just a few plaques but some
individuals with moderate-to-severe psoriasis may have several plaques covering large areas
of their body. On the scalp of patients with psoriasis, the hair traps the scale, resulting in
thicker plaques. Psoriasis can affect the nails resulting in changes such as onycholysis
(separation of the nail plate from the nail bed), thickening, pitting, ridging and salmon-pink
areas.
Psoriasis is associated with psoriatic arthritis in up to 30% of cases. Psoriatic arthritis can cause pain, swelling, stiffness and deformities of one or more joints.
How is scalp psoriasis diagnosed?
Scalp psoriasis is a clinical diagnosis; in other words, it can be recognised by its characteristic
appearance and distribution.
How is scalp psoriasis treated?
The treatment of psoriasis may include:
- Topical treatments i.e., those that are applied directly to the skin
- Phototherapy (although this may be difficult on the scalp)
- Oral medications e.g., acitretin and apremilast
- Systemic immunosuppressants e.g., ciclosporin and methotrexate
- Janus kinase inhibitors e.g., deucravacitinib
- If there is severe body involvement, patients may require biologics e.g., adalimumab, infliximab, ustekinumab, secukinumab, ixekizumab, guselkumab, tildrakizumab and bimekizumab.
Psoriasis
Psoriasis is a common skin disease affecting 2% of the population. It occurs equally in men and women and can begin at any age. Psoriasis is a long-term condition which may intermittently flare up throughout one’s lifetime. Psoriasis commonly affects the scalp. It can affect the nails and the joints as well as the skin.
Psoriasis, particularly moderate-to severe-psoriasis, is associated with an increased risk of anxiety, depression and harmful use of alcohol. Moderate-to-severe psoriasis increases the risk of heart disease and stroke and treatment of psoriasis may reduce this risk. Psoriasis can al-so be associated with diabetes, obesity, inflammatory bowel disease, venous thromboembolism, high cholesterol and hypertension.
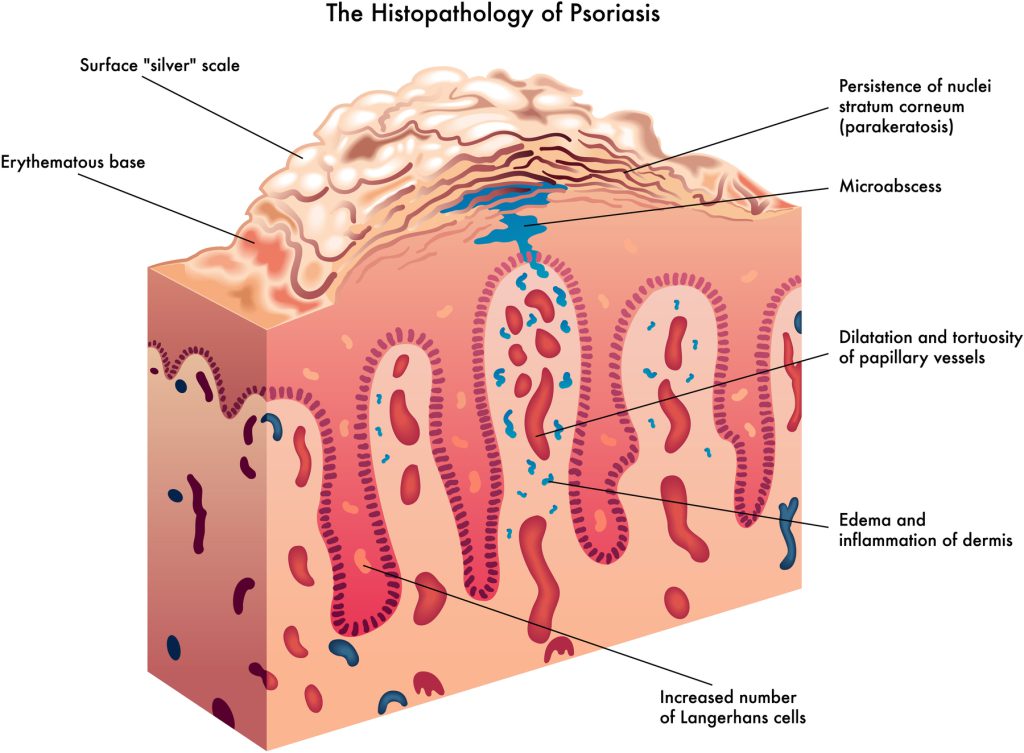
What causes psoriasis?
Both genetic and environmental factors play a role in the development of psoriasis. Infections, stress, damage to the skin and alcohol may trigger flares of psoriasis. Certain medications e.g., β-blockers and lithium can trigger flare-ups of psoriasis, whereas sudden discontinuation of oral cortico-steroids can trigger or worsen psoriasis. Obesity and smoking are asso-ciated with a poor response to treatment. Psoriasis is more common patients with a positive family history. The mode of inheritance is complex and not completely understood.
What causes psoriasis?
Psoriasis may not have any associated symptoms, although itching can occur. The scalp can be particularly itchy. Psoriasis causes well-defined and slightly raised pink or red areas with silvery-white scales (known as ‘plaques’). Many people have just a few plaques but some individuals with moderate-to-severe psoriasis may have several plaques covering large areas of their body. On the scalp of patients with psoriasis, the hair traps the scale, resulting in thicker plaques. Psoriasis can affect the nails resulting in changes such as onycholysis (separation of the nail plate from the nail bed), thickening, pitting, ridg-ing and salmon-pink areas. Psoriatic arthritis can cause pain, swelling, stiffness and deformities of one or more joints.
How is scalp psoriasis diagnosed?
Scalp psoriasis is a clinical diagnosis; in other words, it can be recog-nised by its characteristic appearance and distribution.
How is scalp psoriasis treated?
The treatment of psoriasis may include:
- Topical treatments i.e., those that are applied directly to the skin Phototherapy (although this may be difficult on the scalp)
- Oral medications e.g., acitretin and apremilast
- Systemic immunosuppressants e.g., azathioprine, ciclosporin and methotrexate