Dermatomyositis
Dermatomyositis is a rare condition which causes inflammation in the skin and muscles. In rare cases, only the skin is affected.
What causes dermatomyositis?
The exact cause of dermatomyositis is unknown. However, we do know that it is an autoimmune disorder. A
quarter of adults with dermatomyositis will have an underlying malignancy.
Dermatomyositis affects women more commonly than men. While dermatomyositis can occur at
any age, even in children, it is more common in adults over the age of 50.
What are the symptoms and signs of dermatomyositis?
Dermatomyositis affects the skin and muscles. A rash usually appears before muscle weakness
starts but some patients may only develop a rash.
Dermatomyositis usually affects the muscles involved in movement of the neck, arms and legs. Inflammation results in muscle weakness, stiffness, pain and tenderness.
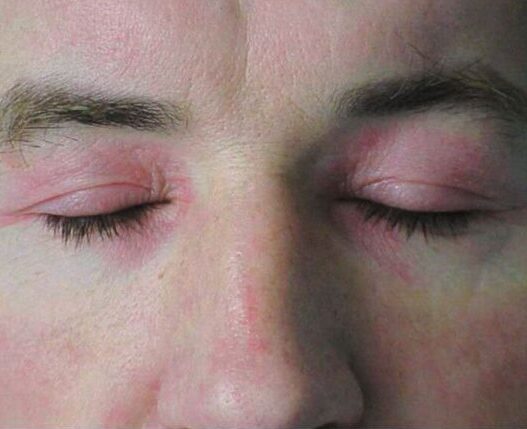
The rash of dermatomyositis can be variable but may affect the area around the eyes (heliotrope rash), over the knuckles (Gottron papules), on the face and the “V” of the neck. It is usually red or purple in colour and can be very itchy, particularly when the scalp is affected. The fingernails may be ragged and the skin around the fingernails may be inflamed. The rash is often made worse by sunlight and is therefore more obvious on areas of the skin which are exposed to the sun.
Dermatomyositis may affect other organs including:- Oesophagus: if the muscles of the oesophagus are affected, patients can experience reflux which causes heartburn. More severe involvement may impair swallowing.
- Lungs: if muscles of the chest wall are affected, patients may develop shortness of breath Sometimes the lung tissue may be affected resulting in stiffness of the lungs.
- Heart: cardiac involvement in dermatomyositis is rare. If cardiac muscle is involved, patients may experience palpitations and lightheadedness.
- Calcinosis: this refers to the presence of firm yellow or white deposits of calcium in the skin and sometimes the muscles. If the deposits become or impair movement, surgical removal may be required.
How is dermatomyositis diagnosed?
- If dermatomyositis is suspected, investigations may include:
- Blood tests e.g., muscle enzymes and autoantibodies
- Skin biopsy
- Electromyography
- Muscle biopsy
- Lung function tests
- Magnetic resonance imaging scan
How is dermatomyositis treated?
The treatment of dermatomyositis may include:
- Sun protection
- Oral corticosteroids
- Systemic immunosuppressants e.g., azathioprine, ciclosporin and methotrexate
- Intravenous immunoglobulin
- Biologics e.g., rituximab